As the world moves towards the recovery phase of the COVID-19 pandemic, airports must put in place effective virus diffusion control measures if they want to stay competitive and reassure both passengers and staff. COVID-19 has increased the perception of health-related risks associated with travelling.
The outbreak has increased awareness of how fast a virus can spread through transport networks, and of the role of airports as important gateways/guardians that can help prevent diffusion into the wider community. It seems inevitable that, just as airports prioritise safety and cybersecurity in their planning and delivery, they will now be prioritising biosafety too.
Airports need to be ready and well prepared for this “new normal” airport experience, a new normal that will have to mitigate the risk of COVID-19 contagion.
What mix of measures should airports implement?
While a raft of guidance for airports has come from relevant bodies to help with equipment choice, or procedures to implement, the decision on the particular blend of solutions is a local one. There is no one-size-fits-all solution.
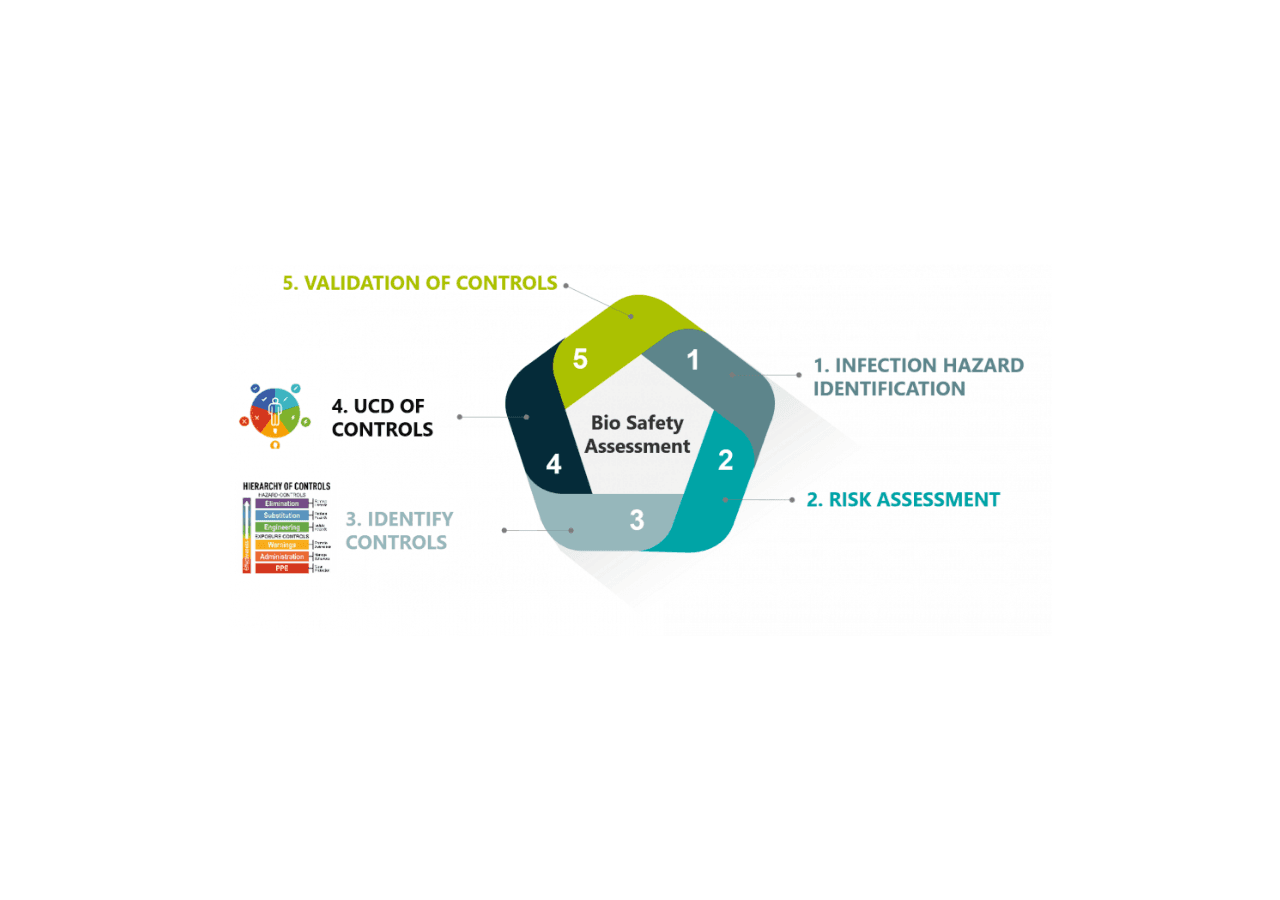
So, before investing in new expensive equipment and new procedures, airports should conduct a bio risk assessment, specific to their environment and operation, so as to identify infection risk for airport staff and passengers across the various airport areas (e.g. check in, security, baggage handling, etc.). From there they can derive a preventive strategy that also takes human behaviour into account.
Our offer.
A bio risk assessment will permit the analysis of the local transmission routes based on specific local conditions (environment distributions, walking paths, layout, equipment, furniture, etc.) and systematic mapping of critical interactions between passengers, between passengers and staff and equipment, and between these user groups and the environment. It is essential to place human behaviours, passenger and staff, at the centre of the analysis as they play a major role in the spread of the virus or in limiting the risks of infection.